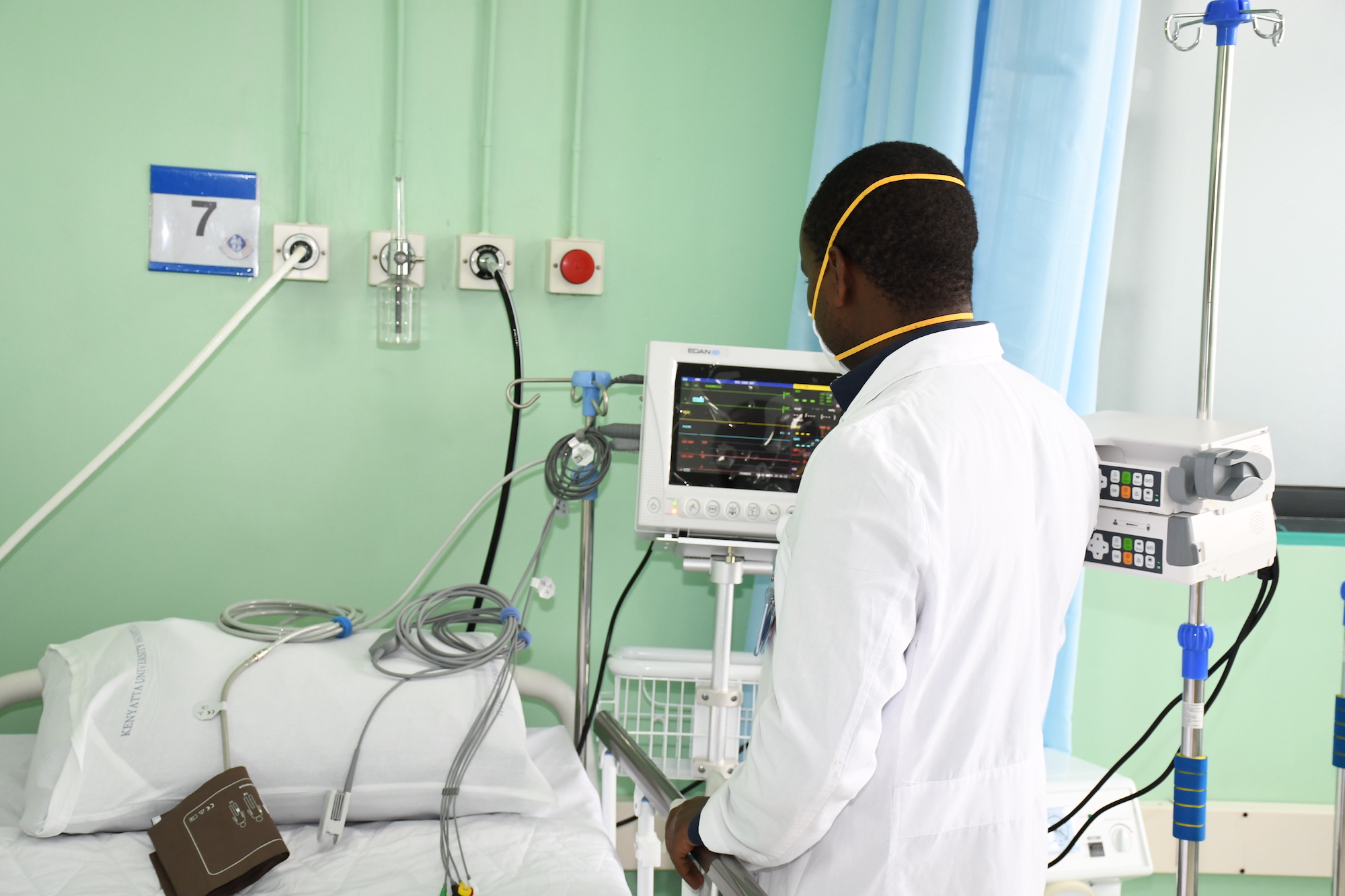
When 90% of women healthcare workers witness sexual harassment and 30% face sexual assault from colleagues, we’re not looking at isolated incidents. We’re staring down a systemic rot that infects Kenya’s medical profession from top to bottom.
New research published in the British Medical Journal reveals what many Kenyan healthcare workers already know but dare not speak: our hospitals and clinics have become hunting grounds for predators in white coats.
The Numbers Don’t Lie
A comprehensive study by the Working Party on Sexual Misconduct in Surgery found that between 2017 and 2022, sexual harassment wasn’t just common—it was endemic. Nearly every woman in healthcare witnessed it. Three out of ten experienced sexual assault directly.
These aren’t faceless statistics. They represent your sister working night shifts at Kenyatta Hospital, your daughter training to be a nurse in Eldoret, your mother serving communities in rural dispensaries.
Why Victims Stay Silent
The research, led by Rebecca A Fisher and including experts like Professor Carrie Newlands, exposes a chilling reality: most victims never report their attackers. The reasons are predictable and infuriating.
Fear of career sabotage tops the list. When your supervising doctor controls your residency, your references, and your future prospects, speaking up becomes professional suicide. The medical establishment protects its own, especially when “its own” are senior male doctors with connections that reach the highest levels of healthcare administration.
Then there’s the blame game. Victims face questions about their clothing, their behavior, their professionalism—everything except the conduct of their attackers.
The System is Rigged
Current reporting mechanisms serve the institution, not the victim. Internal investigations often become exercises in protecting the hospital’s reputation rather than seeking justice. Victims find themselves isolated, facing legal teams and administrative machinery designed to minimize institutional liability.
The researchers propose a national anonymous reporting system—similar to fraud hotlines that already exist. This isn’t revolutionary technology. It’s basic accountability that other sectors have implemented successfully.
What Needs to Change Now
First, Kenya’s medical boards must establish independent investigation processes. No more internal committees protecting colleagues. No more hushed settlements that allow predators to move between institutions.
Second, professional licensing bodies need teeth. Doctors who sexually assault colleagues should lose their licenses permanently, not receive quiet transfers to new hunting grounds.
Third, medical schools must integrate comprehensive training on professional conduct, consent, and power dynamics. The current system produces technically competent doctors who are ethical disasters waiting to happen.
The Real Alarm
The truly alarming reality isn’t the rising number of reports—it’s how few cases actually get reported. When the system punishes victims and protects perpetrators, silence becomes survival.
Every unreported assault, every ignored harassment complaint, every victim who changes careers rather than fight the system represents a failure of medical leadership at every level.
Kenya’s healthcare system already struggles with brain drain, inadequate funding, and public mistrust. Sexual misconduct by medical professionals deepens every crisis while creating new ones.
The medical profession demands trust from patients and society. That trust becomes meaningless when doctors can’t even ensure the safety of their own colleagues. Until healthcare institutions take sexual misconduct as seriously as they take medical malpractice, patients have every reason to question whether their doctors deserve the respect they demand.